
According to my blog publication schedule, this post is supposed to share more information about Chiang Mai, Thailand. However, if you’re a Baby Boomer, you’ve inhabited this planet long enough to know that Woody Allen had it right when he said, “If you want to make God laugh, tell him about your plans.”
My latest trip was not planned. My husband, Steve, and I recently had our first dinner guests since arriving in Honolulu six weeks ago for his three month sabbatical at the University of Hawaii Cancer Center. I kept dinner real simple uncomplicated — rotisserie chicken, salad (with mango as the surprise ingredient) and rice pilaf — courtesy of a box. (I don’t believe in re-inventing the wheel). For dessert — “adult” ice cream sundaes with local macadamia chocolate chip shortbread cookies.
We were having a very pleasant evening—appetizers on our lanai with ocean and Diamond Head views and then dinner. Conversation flowed and everyone was a member of the Clean Plate Club. As we were determining who might want coffee with dessert, I felt the first twinge of what I identified as an incipient GERD (gastro-intestinal reflux disease) attack — heartburn, in layman’s terms. I excused myself and took a dose of my go to GERD remedy — maalox. I was dining with 3 medical professionals. They felt badly I wasn’t feeling well, but no one, including I, was alarmed. The pain was bad enough for me to skip my favorite dessert. While the others enjoyed their ice cream with kahlua or amaretto, I settled for an over the counter acid reducer.
We bid our guests adieu and I retreated to our bedroom to wait for my symptoms to subside while Steve (a truly good guy) washed the dishes. My GERD had been under good control since leaving my more than full time lawyer job. Infrequent twinges were readily controlled with over the counter antacids. The symptoms didn’t subside. They intensified. Steve says I have a high pain tolerance — he has seen me endure kidney stones, child birth and severe GERD attacks without whimpering, even when my pulse rate and blood pressure reading confirmed my pain rating at 9 on a 10 point scale. (For me, 10 is childbirth). He was clear I was in serious pain when I told him I needed to go to an emergency room, the only place I knew I could get the “GI cocktail” of fast-acting medications that can stop the pain associated with a major GERD attack. He was particularly impressed when I said I couldn’t even walk to go outside and take a taxi to the hospital.
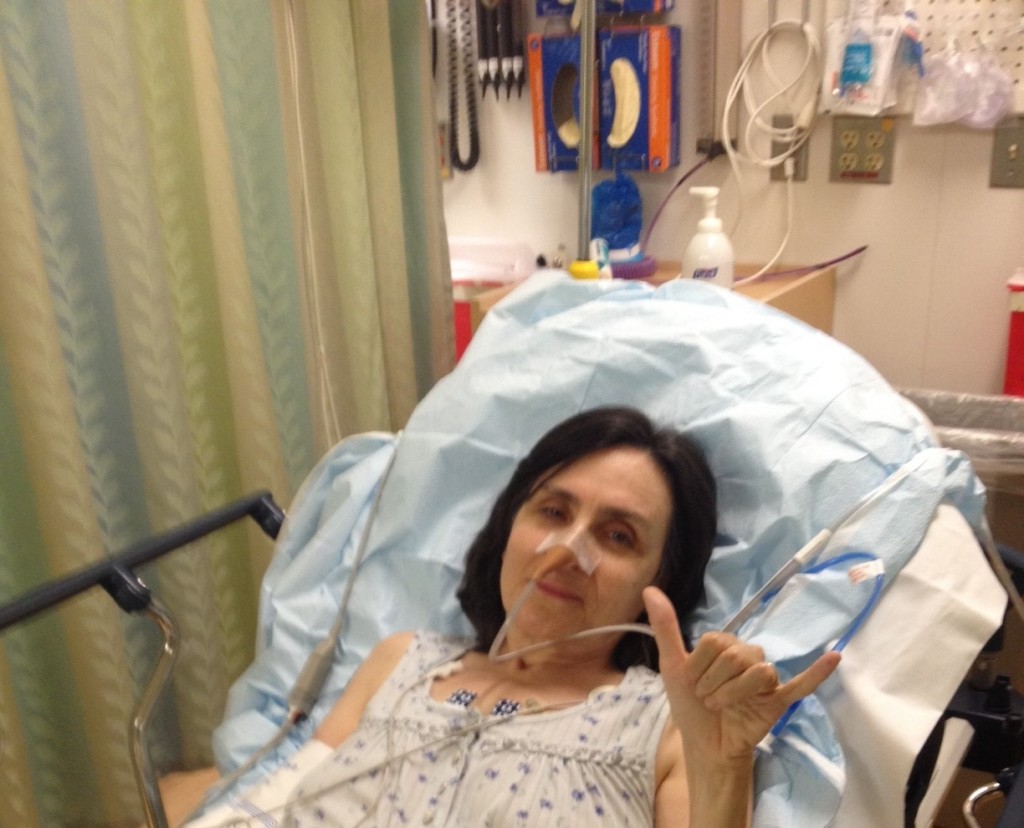
Honolulu Emergency Medical Services (EMS) showed up within five minutes. The two paramedics were extremely professional and thorough. They took us to Straub Hospital, suggesting that I’d likely be tended to more quickly there than at the large tertiary care hospital. I really appreciated that they dispensed with sirens and flashing lights once they determined I was unlikely to flat-line on their watch. They rolled me into the triage area while Steve was dispatched to tend to the paperwork. (Even in Paradise, someone has to pay the hospital bill). Within minutes, the charge nurse introduced himself and started taking my history. He looked like a marine. It turned out he had been a marine. He seemed immensely competent and in command. Steve and I both expressed our opinion that based on previous experience, this was a severe GERD attack that could be stopped in its tracks by a combination of an antacid, a topical pain killer and an antispasmodic. Nurse Marine was willing to entertain that hypothesis, but appropriately, he also wanted to rule out an acute cardiac event. Once I had a normal EKG and had blood drawn, I finally got the elixir I thought would take away my pain. Only it didn’t. Ruh roh.
Eleven Things I Learned after I Found Out I Wasn’t Having a GERD Attack:
1) Bedside ultrasound can be a valuable diagnostic tool in the ER. It told my attending physician that I did not have gall stones, but that I had something that warranted further investigation by a CT scan.
2) You can get an emergency CT scan in the middle of the night at Straub Medical Center in Honolulu. The CT scanner machine will even talk to you! While the Straub radiologist is at home fast asleep or whatever, your digital scan will be sent winging off into cyber space to be read by a radiologist on the mainland who will diagnose a partial small bowel obstruction —- a What? Why? How?
3) Once they know what’s wrong with you, you can have pain meds. Even if you’re allergic to morphine, they have other nice narcotics, like IV dilaudid. If you’re in severe pain, narcotics don’t make you feel high. They just relieve your pain. You are very thankful.
4) The initial treatment for a partial small bowel obstruction is a naso-gastric (NG) tube. The nurse will warn you that getting a plastic tube inserted through your nose, down your esophagus and into your stomach is really quite “unpleasant”. He will say this several times. He will be 100% correct — and then some. Your physician husband will decide he really doesn’t need to see this and will wisely decamp to the waiting room. You realize that freaking out will just prolong the agony and perhaps cause you to end up with a tube in your trachea instead of your esophagus, so you somehow suck it up (literally) and resolve to be a help, not a hindrance.
5) Once the NG tube is in place, you can be transported to your room. You will be very happy to learn that Straub Hospital has all private rooms. You’ll meet your very nice nurse who will explain that the plan of care for your small bowel obstruction is the NG tube, no eating or drinking and IV hydration.
6) It will now be 3:00 a.m. You are aware of all sorts of noises — suction, an IV pump and what you are convinced sounds like a cockroach walking across the pillow behind your head. You will ask your nurse if there are any cockroaches in the hospital. She’ll hesitate and tell you she saw a dead one once. Your husband will decide you’re appropriately psychotic from all you’ve been through and will patiently explain that he doubts very much that you are hearing a cockroach on your pillow. You will be very tired. Swallowing will be very painful. You will decide to let the cockroach thing go.
7) You will fall in love with your husband all over again when you look over and see he is planning to spend the rest of the night on the semi-reclining chair at the foot of your bed. You’re exhausted. You sleep fitfully in between very painful swallows.
8) You will decide that describing the events of the rest of the day would definitely be TMI (too much information). Let’s just say: It. Was. Not. A. Fun. Day.
9) You will send your husband home to get some sleep and spend a second fitful night, partly because you’re in the hospital and partly because your IV pump runs dry twice, emitting a suitably alarming alarm sound. You will learn there’s a shortage of “normal saline” IV solution, so the nurses have been ordered to use every drop.
10) You will find out that your diet (or rather, your lack of diet) has been advanced to clear liquids. You will actually enjoy some beef bullion and red jello for breakfast. When you tolerate this, they will advance you to a regular diet for lunch. A half an egg salad sandwich never tasted so good. When it appears this is on its way to being digested, you will be given the good news that you can go home as soon as transport brings up a wheel chair. You don’t need a wheel chair, but that’s hospital policy, so you cooperate and are deposited at the door in a wheelchair.
11) You will walk back out into the world, whereupon you will feel immensely grateful for modern medicine, that you are no longer in pain, that you married a good great guy, that this didn’t happen when you were in Laos or Cambodia, and that so many people cared enough to wish you well. You will think about and endorse what your 89 year old mother always says, “Any day you can walk out your front door, is a good day.”




{ 128 comments… read them below or add one }
Glad to see that there weren’t any black n’ blue marks on your IV’d arms. So very relieved that all is well again. Ahhh, the things you do to get a new twist to a story!
Thanks, Neva. I guess it is sort of “sick”, but once I could concentrate again, I found myself saying, “Well, at least maybe I’ll get a blog post out of this.”
I’m so glad it worked out OK for you, Suzanne.
I’ve not ended up as a hospital patient while away, but I have ende up on medical clinics in Mexico, Cuba, and Hawaii on previous trips. The reason? Swollen ear wax. It seems my ear wax is prone to swelling in salt water! I therefore have to be sure to get my ears checked before I head to the tropics to be sure I have no accumulation of ear wax before swimming in the ocean.
Doreen, you’re lucky you’ve figured out what was causing your ear problem when traveling. What’s somewhat disconcerting is that we’re not sure what caused my problem, so I sort of feel like I have the Sword of Damocles hanging over my head. I’m hoping that if there is no recurrence, I’ll regain my fullblown wanderlust.
Your #10 brought tears to my eyes…as much as you went through a horrific thing, you are alright, you were within reach of fantastic medical care and your sweet husband was by our side. I’m so glad you’re doing better!
Yikes –
Yes, I think I’m happy this happened to you in Honolulu, which would feel a little more like “home” than SE Asia! So good timing there 🙂
But aren’t we funny that rather than trouble the company that would maybe know it was time to head to the hospital *now* rather than waiting till after the washing up was done we put on a brave face and soldier on until we really can’t move!
So pleased you’re now home – And can hopefully get to the bottom of it over time.
One problem for people who are not overly demonstrative when in pain — even great pain — is that others find it it difficult to guage the extent of the emergency. Steve and I have also had some really unpleasant times with loved ones in emergency rooms (in our hometown–where Steve works even), so our inclination is to hope we can avoid the trip.
Marilyn, as unpleasant an experience as this was, it reminded my husband and me how much we mean to each other — something that can sometimes get taken for granted in our fast paced everyday lives.
Glad you are OK. How terrible to have this happen in Hawaii. Hope this NEVER happens again.
Suzi
Thanks, Suzi. I’m definitely with you on the never happening again thing, but if it had to happen, I’m grateful that it happened in Hawaii where the hospital staff speak English and they are up to date with medical knowledge and equipment. This would not have been the case for the entire month we were traveling in southeast Asia.
You have such a positive attitude, Suzanne! Sick in Paradise is definitely a nasty deal, but you turned it into a great post. Every time my husband and I fly off on an adventure we keep our fingers crossed. But you’re right, God has quite a sense of humor as I found out when I fell and crushed my finger on a perfect beach in Puerto Vallarta, and required surgery.
Thanks for stopping by, Susan. I guess the message here is to expect the unexpected, but to try not to be paralyzed by the fear of it.
Ah ha, so when you commented on the picture of the CT scanner that I posted on FB – that’s what you were referring to. Sorry you had such an up close and personal experience with it! I didn’t want to ask you but thanks for sharing. Glad you are feeling better.
Merryl, I know there’s radiation involved, but I must say, the CT scanner experience is soooo much better than the MRI experience, but they both beat exploratory surgery hands down!
I can’t believe you wrote such an amazing blog with what you’d been through! Kudos! So happy that you’re okay…and that it happened in the US – and not during your travels.
Thanks, Michelle. I think I felt like I wanted to get the story down and other than that my brain was too fuzzy to focus, so I wrote it. I wasn’t sure about actually publishing it, but with some encouragement, I did.
Happy things worked out and like you said you were in Hawaii rather than Cambodia . What an ordeal!
Now that I’m home, in retrospect, it doesn’t seem that bad. I think human beings cope with pain at that level with an element of amnesia. This is why there are any second children being born.
Suzanne,
Life happens and I know you thought profusely about “sharing” this incident through your blog. It is sometimes more than fate I believe, these situations occur within a short distance of wonderful facilities. My heart attack, on my 25th wedding anniversary day transpired 10 blocks from one of the best heart hospitals in the country. I am glad that your husband was there to support you and that the “Marine” kept looking until he discovered the real issue. I am very sorry that you had to endure the NG tube, but glad they had the narcotics to ease your pain. I knew you were a tough lady, but this sounds substantially traumatic at best. I am happy you are back on your feet and out in your tropical paradise again!
Mike
Thanks, Mike. We had something like your experience in our family too. My parents were in Washington, D.C. (visiting from Philadelphia) and they were standing in line to enter an exhibit at a museum. (Dad was an art teacher). My father had a heart condition and collapsed — right in front of the Chief of Cardiology at GW Hospital. The guy didn’t wait for an ambulance. He took my father there in a taxi. Even more remarkably, he was one of the few cardiologists in town that day. Most of them were away attending a national conference.
So glad you are ok and very glad you wrote the blog post … Yes, it was personal but it was about a journey, and beneath the very real pain you managed to bring in a touch of wry humour 🙂 stay well!
Thanks, Johanna. So far, no one has said, “What possessed you to write a blog post about this?” Or, maybe those people just keep that sentiment to themselves!
Suzanne, you turned a terrible experience into a fun read. It is lucky it happened in Hawaii as opposed to Asia. While the caliber of medical care may be good (don’t know) it’s comforting, when in extreme pain and distress, to be able to communicate with the medical staff. Glad they were able to fix this without surgery. I sometimes think about living in South America and then think about medical issues. It sure gives me pause. Thanks for sharing your personal journey.
Like you, my Steve doesn’t make a fuss when he’s ill. He once cooked BBQ for 8 and went to our bedroom. When I got there he said, I think I need to go to the ER. Turned out he was having a heart attack- but everyone ate well that night.
Depending on where you are in South America, you can find pretty decent medical care these days, especially in the capital cities. Some of the docs have even trained in the US. My Steve has never had to spend the night in a hospital (on the receiving end). He told me that if he had as much pain as I did, he would have been screaming like a banshee. I hope we never have to find out if that’s true.
Wow! what an ordeal. So glad you’re better and it wasn’t a heart issue. Your writing was excellent. I loved the 10 points and addition of humour in a not-so-humorous situation. Be well and enjoy paradise. 🙂
Thank you, Suzanne. I’m even more appreciative of Paradise now than I was before the, um, incident. I was able to go to the Bishop Museum today. That should produce a much less dramatic blog post.
Oh my! What a trip! And such a cleverly told tale. Glad you are well!
Hi Suzanne – just caught up with your last couple of blogs. As always, they were absorbing. Pleased you’ve made a full recovery.
Agreed childbirth comes top of the shop on a scale 1 – 10. And you’re so right about appreciating the one you love. Often we need ‘a difficult moment’ to remember how important our partners are.
Keep on blogging Cx
Shrewsbury, UK
Thanks, Chris. I enjoyed following your recent trip to Fort Lauderdale on Facebook. It’s quite amazing how in touch we can be these days across the miles.
I so feel for you ending up in hospital. I am however glad you are OK. Glad you blogged on it. My 8 year old spent 2 days in a Bolivian hospital with blood on the walls, no toilet paper or fresh water, no windows (Xray film) and cardboard to hold up the mattress where springs were missing. Glad you were in a good place to be treated. It must have been very stressful!.
Yikes. I can’t imagine that scene. You must have been worried beyond beyond.
Suzanne – so glad you are feeling well. And, when you walked back out into the world – you were in HAWAII!! Please keep the rest of your trip medically uneventful!
Best thing is… it’s over and your sense of humor is intact!
I think we sometimes use humor as a defense mechanism — like in this situation. 🙂
YIKES. Glad you’re okay.
No,I never worry about medical care because it’s generally good. I’d actually trust the doctors in Thailand a lot more than back home in Australia, my husband had wonderful care when he had surgery there. The kids do take us to A&E rather more frequently than I’d like, on 5 continents now! I’m currently in bed with a painful gall bladder and referred pain to my shoulder, hope it will pass uneventfully! Glad you’re OK, what a horrible thing. I’ve never, ever been in hospital, I don’t want to start!
I wasn’t worried about finding good medical care in Thailand. They have a booming medical tourism industry and our travel doctor told us we’d be fine if we needed medical care there. Laos. Not so much.
I am so terribly sorry for this experience, Suzanne! I’m deeply thankful that it wasn’t something more serious…granted this can become quite serious, very quickly. VERY glad you are feeling better and no more of these for you please! I’ve never had an NG tube but did have to tube patients when I was a medic. No bueno for them. I love that Steve wanted to sleep in the recliner at your side. That me an, “Awww…” moment with a smiling sigh. And don’t knock a fun Code 3 run until you’ve tried it! 🙂
When you were learning to “tube” people, did you ever have to do it to yourself? The former marine nurse who admitted me said that’s how he learned. (Shudder.) As for a “Code 3” run, I’m assuming that means sirens and flashing lights. No thanks. I felt like enough of a spectacle being loaded into the ambulance.
It’s horribly frightful to be doubled up in pain, whether you are home or traveling. Glad this had a good ending and that you felt secure being in good hands.
xo
I think the worst would be having a situation like that if you were traveling alone, in a country where you didn’t speak the language and couldn’t even read the alphabet. I think the moral of this story is that at a minimum, one should probably have medical evacuation insurance. Our home medical insurance would reimburse us (eventually) for medical care in a foreign country although we’d have to front the cost — but in most countries, that’s a lot less than it would be in the US.
The best laid plans of mice and marines ! Great that you came through it with such a positive attitude and took a comedic approach to dealing with a near tragedy. I have never given a thought to medical facilities when travelling. In part because what needed to be done needed to be done and in part because I agree with Woody on this one ! Had a few minor injuries over the years while travelling and generally received good care though there was one location where I decided that the sanitary standards made it a better bet to stitch my own wound. Turning down Amaretto sounds a lot more serious. Hope you will rectify that at the earliest !
Paul, I’m with you on the Amaretto, but I’m still afraid to test myself with that demon alcohol.
Glad you are ok now. Two years ago I fell and broke my arm in Cusco Peru. Was taken to a private hospital and operated on for two hours. Spent two nights in hospital then continued on our trip for another 5 weeks. I was pleasantly surprised how nice the hospital was and had extremely good care. The most important thing here is that you MUST have travel insurance. If I had not had travel insurance I would have gone to the local public hospital and my experience would have been very different.
You could still probably have gone to the private hospital by paying the cost of your treatment up front and then being reimbursed by your travel insurance in the US (if that’s where you’re from). Still, travel insurance can provide some peace of mind and medical evacuation, if necessary.
Booby,
So sorry this happened, but as I read I thought it was your appendix. Glad it wasn’t. No “foreign” hospital stay, but emergency doctor visit in Johannesburg once. In a single payer (free) medical system I was able to see a doctor almost immediately for pink eye, and was charged Nothing. My business partner spent a night in hospital there, same results -immediate service with no charge.
THAT is most definitely a midlife journey!
Oh, this episode does not sound fun! But I suppose you felt like you needed to blog about it? That part amazes me, the willingness to share.
By the way, the expression you were quoting is really Woody Allen mistranslating (retranslating?) this: Der Mentsh Trakht Un Got Lakht – my friends say this often, as does my mother-in-law who is a master at Yiddish.
Years ago I got sick in Israel at age 17. I didn’t end up in the hospital, but I did end up going home early. Not fun. And don’t expect a blog post about my experiences.
Leora, funny you should mention the willingness to share. I wasn’t sure about that, so I posted that question on a boomer travel blogger FB group to which I belong. The consensus there was overwhelming that I should publish this post. A while back, I made the decision that I would interact with my readers as friends or at least as beneficent acquaintances. I used to consider myself an introvert. I guess I need to reassess that self-label.
I’m so sorry to hear that you were so sick and in so much pain. I am glad this happened in paradise and not some developing country. I came very close to ending up in the hospital while I was on an adventure/humanitarian trip to Tanzania this past summer. I was very scared and of course absolutely miserable! I kissed the ground when I finally made it back to the US after that trip. I’m glad you are feeling better and hope your good health continues for the remainder of your time in paradise!
For the first time I’m thinking that maybe some experiences might be foreclosed by my age. It’s not that good a feeling.
Yikes! You add a whole new meaning to adventures in paradise!!! So sorry that you went through it, but elated that you GOT through it! AND got a blog post to boot! I have always feared being sick “on the road” as I used to travel extensively…but thankfully it ha never happened to me. Stay well!!!
It is kind of amazing that becoming a blogger has caused me to find a silver lining in bad stuff that happens — it usually has blog post potential.
Oh dear, do get better soon! Take care 🙂
Unfortunately getting sick is a part of life whether you’re travelling or not. If you have to get sick away from home it’s reassuring to know that good medical care can be found around the world! We’ve found good medical care from Mexico to several countries in Central America (plus it’s affordable!).
It’s true, Anita. Good medical care is now available in more and more places.
BODY-BETRAYAL!!
This is what happens to Boomers after we take care of our body for our whole life – and out of nowhere BOOMER BODY-BETRAYAL!!
This blog is spot on: a true Boomer story with personal reflections. Love it!!
Not happy you had to go through with this but glad you are on the mend.
Dari, I think that might be a good name for a new blog: BOOMER BODY BETRAYAL.
I’m glad to finally find out how you landed in the hospital — in Honolulu, of all places. We are very lucky to have all of the inventions of modern medicine and the care of competent medical professionals (hopefully). Thank goodness you had both here. Thanks for the recap of lessons learned, but I hope I don’t have to remember them any time soon. Never been to a hospital while traveling, but have experienced urgent care in Maui when the hubby developed a very scary-looking infection on his toe. It was nice to know there are doctors working in paradise, even on a Saturday.
Cathy, I also hope you can just file away the “reminders”, but never have to pull them out.
So glad you are ok, Suzanne! What a scary situation.
Ah, this sounds horrible! I actually ended up in hospital earlier this week and it’s never a good place to be! Glad you’re all okay now though 🙂
Hmm. Maybe Mercury is in retrograde. I hope you’re feeling better.
Okay, I know there was nothing funny about this … but #6 gave me quite the giggle not only because you wrote it well, but because we lived in Hawaii Kai for 1 year and at that time I had waist-length hair (ah to be young) and my greatest fear was that one of those giant flying cockroaches would get caught in my hair. No kidding. I worried about that for a year. And your pillow walking cockroach brought it all back. Seriously, tho, I’m glad you’re feeling well and that you were well-cared for.
Thanks for stopping by. I have actually seen two of those giant cockroaches, so in my pain and narcotics addled brain that night, it didn’t seem beyond belief that I could hear one of those was clomping across my pillow.
I like point #7. Glad you had a loving husband by your side. You are blessed to have him.
You can rest assured that I do not take Mr. Excitement for granted!
Honolulu is a great idea! Best for couples gateaway. 🙂
What an unfortunate experience. I am glad, you are feeling better again, Suzanne. It’s bad, if something like this happens while you are travelling, but you were lucky you had your husband by your side to take care of you. My worst experience was a kidney problem I had in Cape Town once (with a group of 24 people I had to take care of). I collapsed during dinner and spent the most painful night of my life in my hotel room waiting for a doctor the whole night only to be rushed off to hospital after that. The worst part of all this was that I was alone and had to handle all the paper work, take care of my tour group and get myself checked in at the hospital and checked out of the hotel.
Monika, I cannot even imagine how you handled all that while being in terrible pain. I truly appreciated that my husband was there with me. I was not thinking all that clearly.
Good to hear you are okay. Let’s hope you don’t have a repeat any time soon. You were certainly blessed to have hubby by your side. I experienced the Thai health care system in Chiang Mai and Bangkok. Even though I could have done without the 26 stitches in my head, I have to say they do a fantastic system. The doctors and nurses were first rate, and the cost was ridiculously low. Stay well! and enjoy Hawaii!
Good heavens. What happened, Nancie? 26 stitches? In your head? I know someone who is in Bangkok right now for dental care that she can get for half the price than it would be in the US—even with the travel expense taken into account. Our travel doctor told us we would be fine if we needed medical care in Thailand.
Glad things worked out for you, Suzanne. Probably good you went to Hawaii instead of Thailand?:-)
Catarina. We did go to Thailand—and Laos, Cambodia and Vietnam. I’m just lucky my attack waited until we arrived in Hawaii.
Hi Suzanne – so glad you’re well now and that you are now able to blog about it with humour. Enjoyed your post.
Lenie
Suzanne, I tried sending you this earlier, but I don’t think I have iPhones down yet. I’m glad you’re well. I was sick once in India, didn’t have a sweet husband to care for me, and was very worried. I learned a lot about diet and eating! Thank you for your humor and for writing.
I always enjoy your blogging!
Ooh. I wouldn’t want to be sick without a loved one in India.
I never thought about what would happen if I needed medical care when I was away from home. However, I do get travel insurance when I go to Florida for the winter. I have only been to Germany and Italy besides Florida and knock on wood have never required any hospital stays 🙂 Although I know that Europe has an excellent health care system (at least in the area I was staying). Your post certainly has opened my eyes though. Glad it all turned out good for you!
If you have decent medical insurance in the US (other than Medicare or Medicaid), andyou have the money to pay out of pocket initially for medical care, probably the most important type of travel insurance you can have is insurance that will pay for you to get back home by whatever means are necessary. That could be an air ambulance (super duper expensive) or even a first class ticket.
First thing is Im glad you are better. Seconds thing is i like the fact that you used GERD so many times. Third nurse marine is hilarious. Fourth this is a very good write up thank you for sharing.
You are survivor with great sence of humour, Suzanne, wish i could be like you, 🙂 Glad all is over, phew….
I’m so glad you were taken to an excellent hospital like that. I’ve had a couple of experiences with emergency care and also was treated well but so far, knock on wood, it has been at home. I haven’t worried about something like that happening in “strange” countries but maybe I will now.
I’m sorry for giving you a new thing to worry about!
Glad you are better and that Nurse Marine knew his stuff. I am a needle-phobic and had to skip by the picture of the IV. The only time I was in a hospital away from home was when I flew head first off my bicycle in college and was unconscious for 30 minutes and woke up in an ambulance with the sirens going. I survived that one.
Oh dear. 30 minutes unconscious might even count as a brief coma (don’t quote me on that). I was really glad not to hear any sirens when I was in the back of the ambulance because that would have meant either 1) I was having a heart attack or 2) the driver was a cowboy and was increasing my risk of being in an accident on top of my already unhappy state.
What an experience, good thing hubby was there and took you and had this attended to…funny how emergency people know the best centers for certain things when you ask them up front. Get a lot of rest and enjoy the warm weather, hope you get to smell some lovely pikaki or plumerias in your daily excursions Suzanne
Uh oh. Noel, I’m going to have to hie on over to your blog to look for photos of plumeria and pikaki.
I had an experience once in the Carribean and it really made me appreciate my health. I have very bad allergies. I had a rash from head to toe. I was taken to the local hospital and they all kept saying I had a really bad sun exposure. I hadn’t even gone out in the sun. I knew I was getting an allergic reaction. They finally gave me shots of predisone of which I knew would help. After I was released we went to the grocery store and I bought only foods that I recognized in cans. Years later on TV we saw a program about how food is preserved in the islands. They use sulfa of which I am highly allergic. Today I carry an epi pen. I was thankful I had my wonderful husband with me.
S-C-A-R-Y. I wonder how many travelers to the Caribbean are aware of the sulfa food preservative issue. It literally could be a matter of life or death.
Eek! I’m glad you’re okay. Bowel issues are never fun. It’s so scary to get ‘sick’ and realize it’s not your usual ‘sick.’ Your story made me teary – just hearing about the pain and the kindness of the people around you – your great husband for staying with you.
Thanks for sharing your story – I know it was painful for you but I really enjoyed reading about it.lol Another adventure for the boomer.
Oh no. I didn’t want to make people cry. That’s why I tried to inject some humor into what could be perceived as a grim situation. And you are right, everyone was truly nice and professional. I felt that I was in good hands — and yes, I also had my safety vest with me — Mr. Excitement.
I’ve been lucky in my travels thus far when it comes to avoiding medical issues, but a person can never be too sure. My friend (who is 55) was recently hospitalized overnight because she thought she was having a heart attack. Turns out it was a acid reflux attack. She may not have been traveling away from home, but the incident made her more certain than ever to go to a different hospital the next time around.
Jeri, acid reflux really can mimic a heart attack. That’s why the first thing they try to do—especially with people of a certain age — is to do tests to rule out an MI. She might have had changes on her EKG that turned out to be benign, but they may not have had her baseline EKG with which to compare it. I don’t think I’d complain too much about being admitted for observation — just to be sure.
My friend insists on having dessert first because you never know what’s going to happen before you get to the good part. Glad that you’re feeling better!
Christina, your friend is brilliant!
I’m very sorry for what you had to endure, Suzanne, and I’m glad that you are now symptom-free. Did any of the treating physicians recommend that post-discharge steps to diagnose whatever caused the problem or suggest ways to minimize the chances of a recurrence?
I’ve never been hospitalized abroad, but I did go through the unforgettable frustration of trying to effectively communicate with a medical provider with whom I did not share a language when I was acutely ill. Ever since, I’ve made sure that I had access to a directory of local English-speaking physicians while I was travelling.
Best wishes for great health during the rest of your time away from Philadelphia, Leslie
Thanks, Leslie. The only discharge instruction I received was to follow up with my primary care physician, except oops, I don’t have one in Honolulu. My husband emailed a gastroenterologist colleague back at Penn who recommended that I see a gastroenterologist for a work up to see if they can determine what the problem was. I spent some frustrating time on the phone today with a gastroenterologist’s office because they insisted on a referral from my primary care doc. I finally called the surgeon who saw me when I was in the hospital and she did the referral for me. I have an appointment for tomorrow — we’ll see.
Good for you! (I speak as one who also has a high pain tolerance was not diligent about following up on diverticulitis. All ended well, but only after I had emergency surgery. Fortunately, no NT tube required.) I’ll be thinking of you today, Leslie
Glad you shared the story, Suzanne. I was just about to say we’d never set travel plans based on health care or related issues, but then I remembered we canceled a trip to Mexico because of (Tom’s) doctor’s orders. Ended up having a fine time in Orlando, as two grown-ups sans kids!
Over the years of traveling, we’ve had all kinds of health care, all excellent and reasonably priced. That includes England, Spain (house call), and Japan (ER). And my dentist in Minneapolis is from Mexico. Does that count?
Now that you mention it, I did have some work-up for kidney stones in the US before leaving on a trip to Europe to make sure nothing was lurking, ready to ruin our vacation in Europe. It wasn’t that I thought I couldn’t receive good medical care in Belgium, but with a limited amount of time to travel, we didn’t want to spend it checking out the Belgian health care system.
Hello; I travelled a lot with the family’s carnival. I never thought about medical care or lack of it. but after reading this post, now i probably will be thinking about it. I want to travel more for my business. I’d love to travel as much as you have for your blog. I’m sure that the standard of medical care we expect here is higher if not just different from other parts of the world. glad you got such great treatment so quickly and that your husband is one of the good guys. tai care, Max
Hi Max: The truth is that one can receive terrible medical care in the US and great care in another country — it just depends. The problem is that most laypeople can’t really assess the skill and training of the medical professional they’re dealing with. They can judge whether they like a physician’s demeanor, office staff, and even whether a hospital or doctor’s office seems clean or dirty. That’s why I was so relieved to have Steve by my side to keep a trained eye on things. I do hope you have the chance to travel more.
I’m glad that you are ok.
While kicking in the water on the Texas coast I ran my foot up a rusted out broken wire coat hanger. We were on Port Aransas and our only choice was a small doctor’s office that had and did everything I needed. He was an excellent (and up-to-date) doctor, phew! Although I will say that some of the retired doctors who do an ER stint are a lot wiser than some of the younger ones.
Sort of ruined my running around but I did get to sit on the balcony and do a lot of wonderful reading (without guilt).
I’m glad I found your blog – it is SUCH a relief not to read about diapers, young children or whatever else younger people blog about that snoozes me now.
Yep. Until and unless one of our sons produces a grandchild, you won’t be reading about diapers and young children here. 😉
What a story! I’m so glad you’re out of it in one piece and had the sense of humor to say it’ll make a great blog post. You do have a great husband.
In answer to your question, no, I don’t let the quality of medical care affect my travel decisions, partly because I am over 50 and take zero meds, and partly because I have been very impressed with the foreign medical care I have received and read about. That said, I’m happy to know there are viable options for those of us who don’t handle narcotics well.
Linda, dilaudid is actually a narcotic. After my pain had been relieved to the point that I was pretty sure I wasn’t going to slit my wrists, I was able to be switched to IV toradal which is in the NSAID family (as is ibuprofen (advil) ) and is not a narcotic.
What a spoiler than was, but glad you are Ok Suzanne and managed to write about it too..
Thanks, Welli.
Oh Suzanne, what a nightmare! So glad you are better. I think the sounds at night while you are alone in a hospital bed are very scary. Your husband is amazing and he would not want to be anywhere else but with you. I think these personal posts are endearing. To allow yourself to be vulnerable and share a story like this actually exemplifies great strength. Bravo to you!
I think some people (most people) seem to appreciate the fact that I wrote and posted about this experience. Others are probably rolling their eyes, but, oh well…. it’s difficult to please even some of the people, some of the time.
Any illness I’ve had while traveling has been minor and not required medical attention, but even a minor ailment makes you long for home and wonder if you should stop traveling. I’m glad you were able to get such good and quick care. Hope you’re feeling better.
It’s true. Being sick sucks and being sick away from home, really sucks.
Hello
I feel sad to know about the pain you went through but I am glad that you are fine now.
It’s very hard sometimes in a different country. I feel you are a courageous lady as you have written about your experience. I believe you must have gone through same feelings while writing.
It’s really nice that you got quick care and hospital had good facilities.
I wish you happy and blessed life with a wonderful and caring husband.
Fortunately, Hawaii isn’t it a different country from the United States—although in virtually every state in the U.S., you can have some experiences that make you wonder what country you’re in — if not even what planet you’re on. 😉
Hi Suzanne,
Your story just about sums up “if you want to make God laugh, tell him about your plans.”
Just seeing the picture of Waikiki brings back happy memories for me. I was stationed in Pearl Harbor in the middle 70’s and have subsequently been to Kauai as well. I love Hawaii.
I like your spunk! You thought to help others learn from your ordeal. I wish you healthy and happiness.
Kind Regards,
Bill
There is something endearing about Waikiki even though it’s pretty touristy. Maybe it’s Diamond Head always there in the background. The military had a pretty big presence here with a hotel for active military and their families and the Fort DeRussy Recreation Area.
It was so right to write about your unexpected trip detour! It piqued self awareness and loving support from your husband. Fortunately, your condition resolved without surgery! Love how your story struck a nerve with many others who wanted to share their own.
Unlike 20-somethings, I think Baby Boomers are keenly aware of the stuff that can happen. The key is to not let that be paralyzing.
Comment on Boomeresque 4/5/14
This sounds like quite an ordeal and nothing like a Hawaiian Holiday. If you travel long enough you’ll inevitably get sick en route. If it had to happen I am glad it happened in a place where you could get trustworthy medical care.
Over the years I have had a few health issues while traveling.
I suffered a severe case of the flu in Helsinki, Finland / Kiev, Ukraine. It made the transit between the two cities quite uncomfortable but I bounced back once in Kiev and traveled for another 5 weeks.
I developed vertigo while living in New Zealand, which I at first thought must surely be a brain tumor. For several days I could only walk by bracing on the walls of my apartment or by crawling.
The only thing remotely similar to what you encountered happened to me just prior to leaving on a 10 day snow caving expedition in Idaho. It was only with hindsight that I realized that I had a seeping appendix that flared up just before the group was to begin x-c skiing the haute route. I thought it was just an upset stomach exacerbated by a minor cold and I was determined not to be left behind by my expedition group. Thankfully a couple of earth momma types that were also on the trip with me loaded me up with Golden Seal & some type of boysenberry elixir. The first day of skiing was a bit rough but eventually the Golden Seal Boysenberry treatment cured my cold and with the cold taken care of my immune system subdued the leaky appendix, or so I was told.
It wasn’t for another 2-3 months until I was hit by an attack so severe that I wound up having an emergency exploratory surgery, during which they discovered the leaky appendix had contaminated my entire abdominal cavity with gangrene.
Thankfully the surgery took place back home in Colorado. I feel lucky I made it through the snow caving trip and didn’t wind up buried in a snowdrift somewhere in the Sawtooth Mountains.
The one question I had about your situation is, why is the acronym for gastro-intestinal reflux disease GERD not GIRD?
I’m glad you are getting back to feeling better.
Scary appendix story. GERD stands for Gastro – esophageal reflux disease—not gastro – intestinal; hence, GERD.
What a horrible experience. I’m so glad it got resolved in such a quick, if unpleasant, manner. Hope you’re feeling much better.
I have to say I am generally oblivious about thinking about emergency care when I’m travelling. This will definitely make me reconsider my devil may care attitude.
Oh my goodness, I have been to a hospital when I was on a trip only once, for what I thought was a small irritation of the eye (pink eye). It turned out I had some how scratched my cornea and had a raging infection that was ensuing. I was out of commission for a few days but luckily no serious damage was done. All that said, I am so glad are is right with you and the pain is gone. 🙂
I’ve never ended up in a hospital away from home but I do work in a hospital. In ER too. And as the admitting clerk I’m the one who has to take the insurance and do the paperwork. Six months doing my job and the first thing you say when someone says travel is MAKE SURE YOU HAVE TRAVEL INSURANCE and it’s the first thing you do when planning a trip of your own.
I’m glad you got the care you needed and are feeling better. Hopefully you’ll be back to normal and travelling in not time.
You are SO lucky to have Steve who I am sure, by his presence and credentials, keeps everyone on their toes. Not that I would expect people not to do their jobs effectively, but ya know, “Sh.. Happens!” and I think less “Sh.. Happens” when they know that you or your associate (aka Dr. Excitement) know….just sayin’. On my honeymoon I got turista, but it didn’t necessitate a hospital or doctor visit, just the advice of the concierge at our claptrappish hotel to grate a green apple and mix it with sugar and lime juice, consume said mixture, and voila! I think it worked….or else my fairly mild case just ran it’s course, rather quickly.
BTW I think it was John Lennon who said something similar: “Life is what happens while you’re busy making other plans”…or something like that, of course, said with a Liverpudlian accent!!
My Dad loves Hawaii so much that he went every year for over 10 years and eventually retired there. Beautiful. Summer year-round (for the most-part).
I’m glad this is now history but geesh. How does this happen??????
{ 11 trackbacks }